Hong Kong Researchers Unveil AI Co-pilot System Poised to Reshape Ophthalmic Clinical Workflows
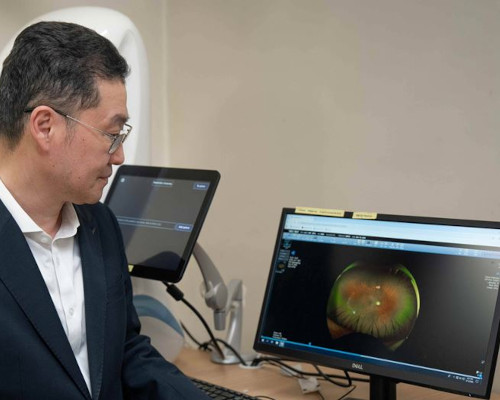 A next-generation decision support platform that goes beyond image analysis could have significant implications for eye care practice globally.
A next-generation decision support platform that goes beyond image analysis could have significant implications for eye care practice globally.
Researchers at The Hong Kong Polytechnic University (PolyU) have announced the development of "EyeAgent 2.0," a clinical-grade artificial intelligence co-pilot system designed to support ophthalmologists and eye care clinicians across the full continuum of patient care: from initial diagnosis through to treatment planning and long-term disease management.
The development comes in response to accelerating population ageing and a growing shortage of specialist doctors, challenges that are placing mounting pressure on the consistency and efficiency of ophthalmic diagnosis across global healthcare systems. Australia is no exception, with ophthalmology regularly flagging among the most wait-listed specialties in the public system and rural access remaining a persistent concern.
From prototype to platform
The PolyU team had previously developed a prototype system called "EyeAgent 1.0," capable of integrating multimodal medical data, including clinical text and images, to provide diagnostic assistance. Pilot testing in hospitals across Hong Kong and mainland China generated positive clinical feedback, paving the way for the more ambitious second iteration now underway.
EyeAgent 2.0 is being built around a domain-specific foundation model trained on large-scale, real-world multimodal electronic medical data sourced from leading ophthalmic centres across different regions. The system will integrate fundus imaging, optical coherence tomography (OCT), angiography and clinical text data.
Critically, the system is not simply another image analysis tool. Through a multi-agent collaborative framework, it is designed to simulate actual clinical workflows, including data integration, differential diagnosis, treatment planning and disease progression prediction, with the explicit goal of moving from one-time image analysis towards continuous decision support throughout the course of disease.
Keeping clinicians in the driver's seat
For practitioners wary of AI encroaching on clinical autonomy, the PolyU team has been deliberate in its framing. The system's design emphasises human-AI collaboration, with AI serving as an auxiliary tool for enhancing data integration and analytical capabilities, while all final clinical decisions remain doctor-led.
Based on current model validation and prototype testing, the team anticipates the completed system will significantly enhance diagnostic consistency and efficiency, while reducing the time doctors spend on case organisation and documentation, helping to alleviate workload pressure in high-volume clinical environments.
A regulatory pathway in sight
Leading the research is Professor He Mingguang, Chair Professor of Experimental Ophthalmology and Henry G. Leong Professor in Elderly Vision Health at PolyU's School of Optometry, and Director of the Research Centre for SHARP Vision. He has outlined a clear commercialisation roadmap.
"Our goal is to develop the system into a 'Software as a Medical Device' compliant with regulatory standards, with plans to progressively advance registration and deployment efforts following completion of clinical validation," Professor He said. The team plans to complete system development and validation within the next two years, followed by productisation and commercialisation.
The system is slated to pilot first in the Hong Kong market before expanding to the Guangdong-Hong Kong-Macao Greater Bay Area, mainland China and overseas markets. Australia, with its established regulatory framework for software as a medical device under the TGA, could be a natural candidate for early international adoption.
Business model and deployment flexibility
The system is intended to adopt a hybrid business model combining annual subscriptions with usage-based charges, and will enable flexible deployment tailored to diverse hospital information system architectures, a consideration that will resonate with Australian practitioners navigating the country's varied public and private health IT environments.
The project has applied for government innovation and technology funding. For Australian eyecare professionals, EyeAgent 2.0 is one to watch; not as a distant hypothetical, but as a system with a concrete commercialisation timeline and the clinical validation work already underway to back it up.